
In a converted storage room at the University of Missouri School of Medicine is a laboratory that could be mistaken for a Hollywood special effects studio. There are heads, arms and legs that look, feel and bleed like the real thing.
These artistic inventions were created from scratch by the Shelden Clinical Simulation Center’s Damon Coyle to give future doctors and nurses better training devices so they can deliver the best possible care to patients.
“I’m able to use my skill sets to make really interesting things that also happen to help people,” Coyle said. “The ultimate goal is to reduce negative patient outcomes.”
The story of this do-it-yourself approach to medical simulation began in 2018. Dena Higbee, the School of Medicine’s director of simulation services, was trying to figure out how to give medical and nursing students the best training without blowing up her budget. A single medical task trainer can cost more than $1,000, and there are many tasks to learn and many students to teach.
“After 20-some years working in medical simulation, I realized there are a lot of products that are on the market that did not quite meet what we wanted for training purposes, and the cost continued to rise on those products,” Higbee said. “When Damon and I connected, I figured out he has the skills to do this, and I have ideas about a lot of the products we want to replace and the disposable pieces we want to make ourselves.”
Coyle’s job title is “simulation innovation specialist.” He has a rare combination of artistic ability, medical knowledge and mechanical handiness. Coyle studied both sculpture and biology as an undergraduate at MU, and he completed three years at the MU School of Medicine before deciding his heart was in art. When Higbee approached him about working for her — part-time at first — to make training devices, he realized it was a perfect opportunity to use his talents for a higher purpose.
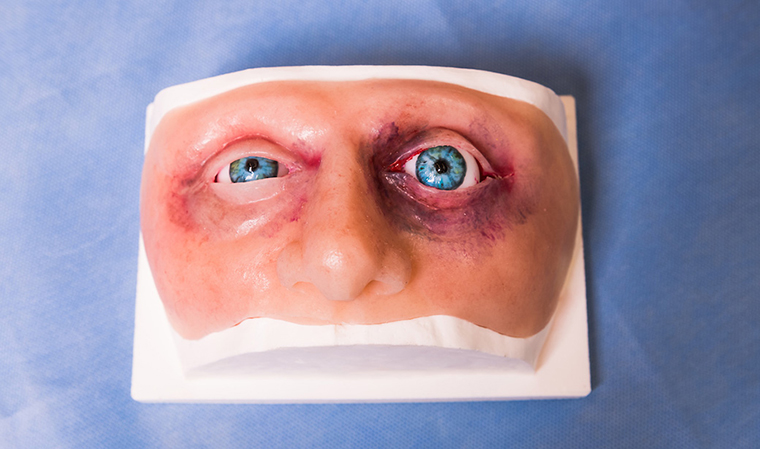
Coyle started by making trainers that MU nursing students could use at home to practice inserting catheters and giving injections. As word got around about his skills, requests started rolling in. Could he make a lifelike model to mimic a hemorrhage … eye trauma … even a C-section? With a few trips to Menard’s for supplies, some trial-and-error in the lab and feedback from the MU experts who would be using the products, he realized he could create a wide variety of realistic task trainers at a reasonable cost.

‘An amazing product’
A good example of a homemade simulation device that has been a huge improvement over products currently on the market is the neonatal IV trainer. One of the most challenging tasks for a neonatal intensive care (NICU) nurse is inserting an IV into the tiny foot or hand of a newborn. It’s so tricky, new NICU nurses often aren’t asked to start a peripheral IV in their first year on the job.
“You get a lot of practice in nursing school sticking adults, who have much bigger veins, but when you come to the nursery, the veins are very small and very difficult to get,” said Christine McQuay, RN, a nursing supervisor in MU Health Care’s NICU. “It takes a lot of practice to build those skills.”
McQuay said there weren’t any simulation devices on the market realistic enough to help nurses learn before making their first stick. So the NICU nursing staff approached Coyle to see if he could build a better baby limb.
He began by having nurses send him photos from the NICU with rulers next to the babies’ arms and legs so he knew the correct dimensions. Next, he sculpted limbs out of clay. He created silicone molds around those sculptures and used the molds to create master models made of hard plastic. He then poured platinum cure silicone around the master models in the mold to create thin, translucent skin. The skin fit over a silicone core that replicates the muscle and bone structure of the arm or leg, with tiny tubes inserted to mimic blood vessels.
His final flourish was a detailed paint job.
“If you look at your hands, you have yellows, greens and reds,” Coyle said. “Those are things we look at and don’t pay a lot of attention to, but an artist does. You would notice if it wasn’t there.”
The result was limbs that look and behave almost exactly like the real thing. McQuay said NICU nurses practice on the neonatal IV trainers once a month, and even the experienced nurses have joined in to sharpen their skills.
“Having the ability to maneuver the hand or foot a certain way to get the vein to pop up and give you the length to thread the catheter gives you the ability to manipulate the hand the way you would in real life to get that IV in,” McQuay said. “The veins are in the same place where you would find them on an infant, which makes it very realistic when you go to stick. It’s an amazing product.”
Ready for market
When Higbee shows her peers at other medical schools the task trainers being made in-house at MU, they are first impressed and then inquisitive.
“They say, ‘Man, this is a lot different than what we’re used to,’” she said. “A lot of these colleagues I’ve known for 20 years, and as we’re able to compare notes on what we’re spending, they ask how they can get ahold of these products.”
Funny they should ask, because Higbee and Coyle are currently working with Brian Buntaine of MU’s Technology Advancement Office to explore the commercial potential of the devices. Buntaine said simulation equipment manufacturers have shown lots of interest in the products, with the neonatal IV trainer attracting the most attention.
“It has the potential to fill a niche in the market that is currently unserved,” Buntaine said. “Many companies offer simulated arms to practice IV access and administration of shots, but none of them provide a simulated neonate arm or leg as realistic as this one.”
Higbee and Coyle are excited about the possibility that products created at MU can help future doctors and nurses around the world to provide better care to patients.
“If we can provide something that looks, feels and behaves real,” Coyle said, “then we can help increase positive patient outcomes.”





