Fewer than 10% of dermatologists practice in rural areas, according to the Journal of the American Academy of Dermatology.
That means primary care physicians (PCPs) are often relied upon to diagnose skin cancers in areas where access to dermatologists is lacking, even though multiple studies have shown most PCPs do not feel adequately prepared to diagnose and treat many skin conditions. Researchers from the University of Missouri School of Medicine conducted a two-year study of the Extension for Community Healthcare Outcomes (ECHO) telehealth program in Missouri and found the program provided participating PCPs with expert recommendations that benefited nearly 84% of adult cases and 72% of pediatric cases.

“When it comes to skin cancer—which is the most common type of cancer in the United States—a timely diagnosis saves lives,” said Mirna Becevic, PhD, associate research professor at the MU School of Medicine. “Given the shortage of dermatologists in rural parts of the country, it is essential that we increase the PCPs skill in identifying patients with a high risk for skin cancer.”
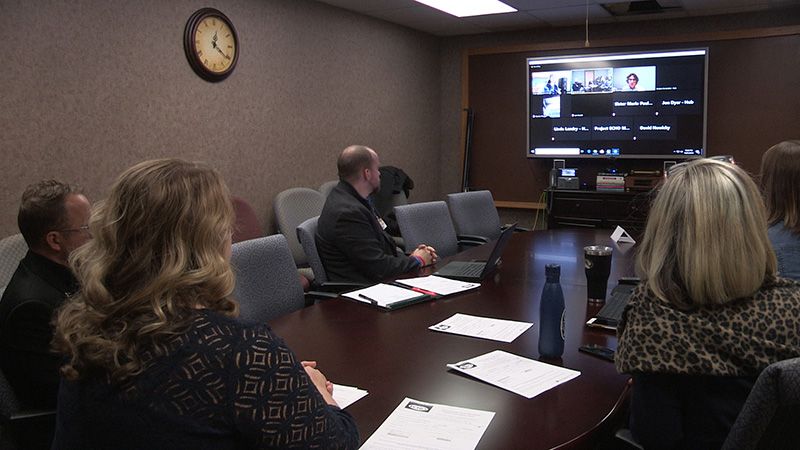
The retrospective study examined 137 adult and 44 pediatric dermatology cases presented between 2016 and 2017 through the University of Missouri Show-Me ECHO Project where 60 PCPs from rural areas across Missouri were linked via videoconferencing with dermatologists at University of Missouri Health Care in Columbia, who provided presentations and expert recommendations on de-identified cases during weekly, hour-long sessions. During those videoconferences, the research team discovered 44% of adult dermatology cases and nearly 28% of pediatric cases were incorrectly diagnosed by the PCP.
“A lot of literature was pointing to the fact that residents and PCPs do not get enough training in dermatology, but a big part of their clinic is skin conditions,” Becevic said. “We wanted to find out how much do the participating PCPs know about skin issues, how accurate are their diagnoses, and how accurate is their treatment? Our study results matched what we knew from the literature––that a majority of PCPs do not feel adequately prepared to diagnose and treat common skin conditions.”

“This program breaks the mold,” said study co-author Jonathan Dyer, MD, professor and chair of the Department of Dermatology at the MU School of Medicine. “These are real cases and real-life discussions. We believe this project will help doctors take the cases presented and apply them to others in their clinic. The patient will benefit from this program because they are provided the correct diagnosis at the correct time, right at the point of care, which will improve their outcome and reduce their cost and the expense incurred by the health system.”
In addition to Becevic and Dyer, the study authors include University of Missouri School of Medicine colleagues Jane McElroy, PhD, professor of family and community medicine; Kathleen Quinn, PhD, former associate dean for rural health; and Calli Morris, medical school student. The research also featured contributions from Catherine Bridges, MD, Children’s Mercy Hospital, Kansas City.
The study, “Utility of Dermatology Extension for Community Healthcare Outcomes (ECHO) sessions in the adult and pediatric population,” was recently published in the Journal of Telemedicine and Telecare. The authors of the study declare that they have no conflicts of interest related to this study.