Nutrition plays a critical role in the prevention and management of chronic disease, yet it has historically been underrepresented in medical education. The University of Missouri School of Medicine is addressing this gap through a comprehensive nutrition curriculum integrated across all four years of undergraduate medical education.
The curriculum is designed around clearly defined competencies and emphasizes foundational nutrition science, clinical assessment, patient counseling and application in real-world care settings. Students develop the skills needed to recognize diet-related disease risk, interpret nutrition-related clinical data- and incorporate evidence-based nutrition strategies into patient care. By embedding nutrition longitudinally rather than confining it to isolated coursework, the School of Medicine is preparing future physicians to address metabolic health and chronic disease with greater precision, consistency and clinical relevance.
“We see a great pivot in the practice of medicine, as physicians increasingly need to focus on health, not just response to disease. A strong and multifaceted nutrition curriculum comes from that vision. With it, we aim to make our graduates irreplaceable in the 21st century physician workforce.”
- Joel Shenker, Associate Dean for Curriculum
Required nutrition curricular content, by student year.
| Hours | Competency Domain |
|---|---|
| M1 Year (AY26/27) – 32 hours | |
| 13.5 | Foundational Nutrition Knowledge |
| 11 | Nutritional Assessment & Diagnosis |
| 4 | Food and Nutrition-Related Communication Skills |
| 7 | Experiential Hands-on Learning (Culinary Medicine) |
| 3 | Medical Interventions in Combination with Lifestyle Practices |
| M2 Year (AY26/27) – 13 hours | |
| 4.5 | Foundational Nutrition Knowledge |
| 5 | Nutritional Assessment & Diagnosis |
| 2 | Food and Nutrition-Related Communication Skills |
| 1.5 | Medical Interventions in Combination with Lifestyle Practices |
| M3 Year (AY26/27) – 14 hours | |
| 2 | Foundational Nutrition Knowledge |
| 1.5 | Nutritional Assessment & Diagnosis |
| 3.5 | Food and Nutrition-Related Communication Skills |
| 5 | Collaborative, Interprofessional, Referral, and Patient Management |
| 2 | Medical Interventions in Combination with Lifestyle Practices |
| M4 Year (AY26/27) – 4 hours | |
| 4 | Experiential Hands-on Learning (Culinary Medicine) |
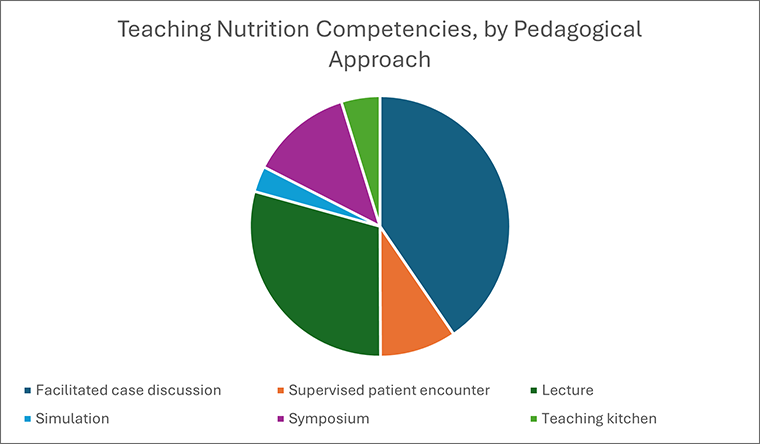
Teaching of nutrition competencies, by pedagogical approach.
| Pedagogy | Percent (%) |
|---|---|
| Facilitated case discussion | 40.5 |
| Supervised patient encounter | 9.5 |
| Lecture | 29.4 |
| Simulation | 3.2 |
| Symposium | 12.7 |
| Test Kitchen | 4.8 |
Nutrition curricular content, by competency.
| Competency Description | Suggested Hours | MUSOM Hours | % Time |
|---|---|---|---|
| Pathological states affecting nutrient absorption | 3 | 3 | 4.76% |
| Principles of healthy balanced diet | 2 | 2 | 3.17% |
| Mitochondrial metabolism & insulin resistance | 4 | 4 | 6.35% |
| Hormonal regulation through food composition | 3 | 4.5 | 7.14% |
| Integrated nutrition status assessment | 4 | 5 | 7.94% |
| Biomarkers for malnutrition risk | 3 | 4.5 | 7.14% |
| Metabolic biomarker interpretation | 4 | 4 | 6.35% |
| Network biology disease assessment | 4 | 4 | 6.35% |
| Lifelong dietary counseling | 3 | 5.5 | 8.73% |
| Motivational interviewing | 4 | 4 | 6.35% |
| Multidisciplinary nutrition care | 2.5 | 2.5 | 3.97% |
| Appropriate nutrition referrals | 2 | 2.5 | 3.97% |
| Personalized meal planning from clinical data | 4 | 8 | 12.70% |
| Teaching kitchen learning lab | 2 | 3 | 4.76% |
| Nutraceutical interventions | 1 | 1 | 1.59% |
| Prioritizing food-based medicine | 3 | 5.5 | 8.73% |
| TOTAL | 63 |
Resources
- U.S. Department of Health & Human Services Medical Education Nutrition Framework
- JAMA: Proposed Nutrition Competencies for Medical Students and Physician Trainees







